Hidradenitis suppurativa (HS), also known as acne inversa, is a chronic inflammatory skin disease that quietly undermines the body’s largest organ.
Far from a simple surface rash, HS originates deep within hair follicles, where blockages trigger relentless inflammation.
This silent internal assault often goes unnoticed until painful lumps emerge, leaving many patients to suffer for years before diagnosis.
Affecting roughly one percent of the population, HS devastates quality of life through recurring flare-ups and permanent damage.
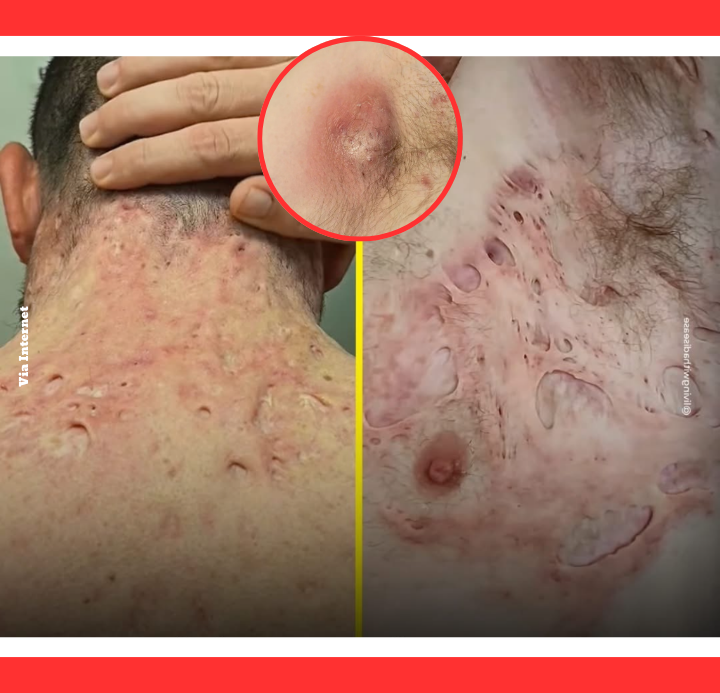
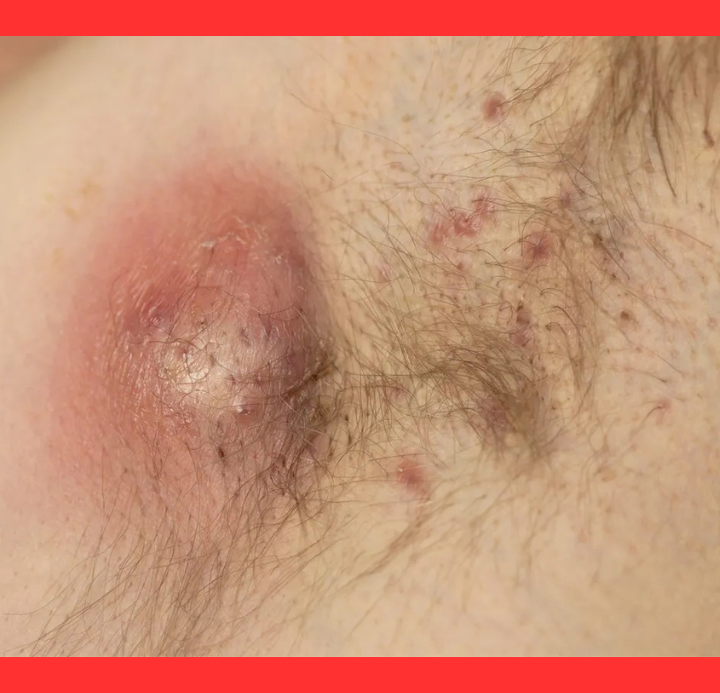
The condition manifests as tender, pea-sized nodules that swell into abscesses filled with pus.
These lesions frequently rupture, draining foul-smelling fluid and blood, then heal with thick scars. Blackheads and double-ended comedones often appear in clusters.
Over time, repeated cycles create open wounds that refuse to close, turning everyday movements into agony.
What begins as an occasional bump evolves into a lifelong battle against pain and infection.
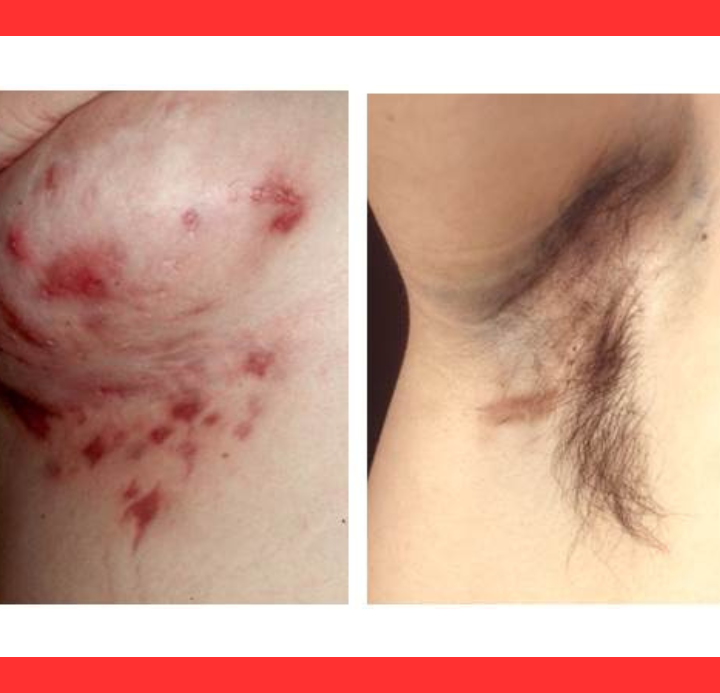
HS strikes areas where skin rubs together and sweat glands thrive: armpits, groin, buttocks, inner thighs, and beneath the breasts.
It typically emerges after puberty, striking women more often than men, though anyone can develop it.
The disease does not discriminate by body type initially, but friction in skin folds accelerates its progression, trapping bacteria and intensifying the hidden war beneath the epidermis.
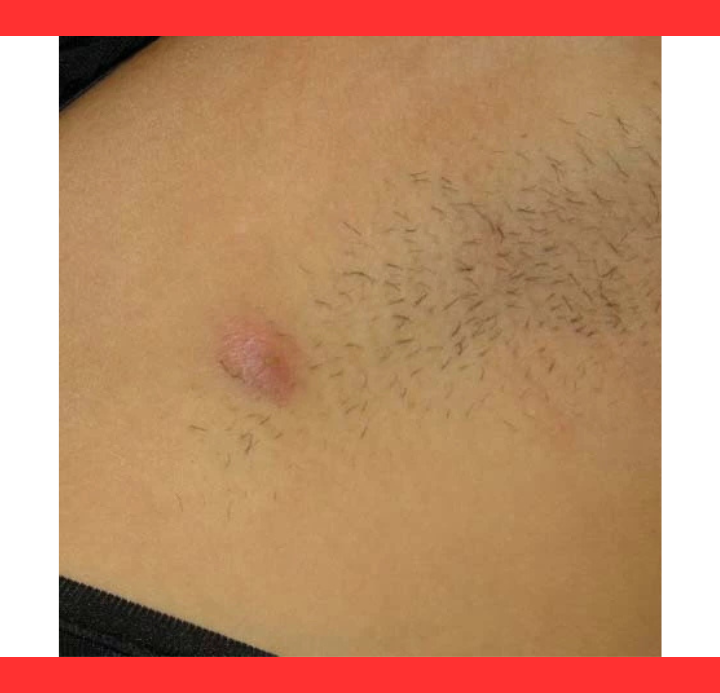
Genetic factors play a major role, with family history increasing risk significantly.
Hormonal fluctuations, especially around menstrual cycles, can trigger flares. Smoking and obesity stand out as powerful environmental triggers; nicotine worsens inflammation, while excess weight heightens skin friction and alters immune responses.
Experts emphasize that HS stems from an overactive immune system attacking hair follicles, not poor hygiene or contagion.
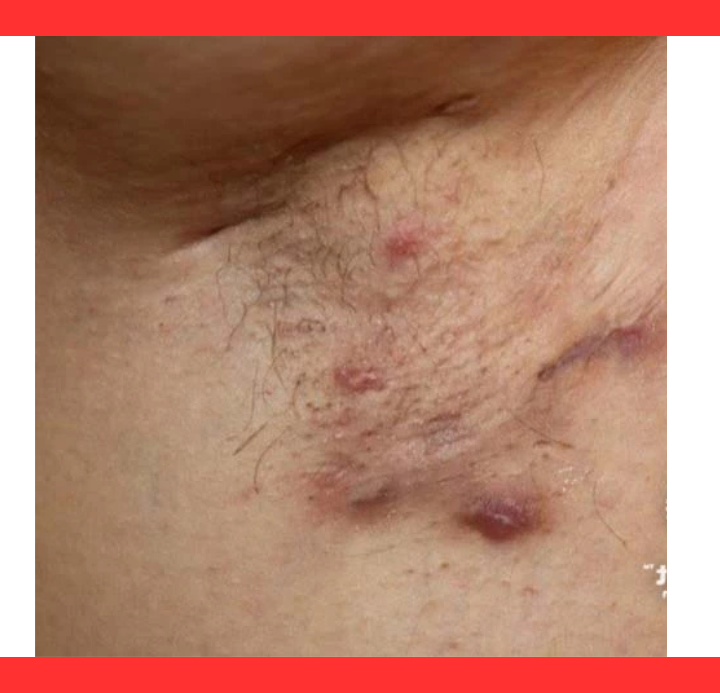
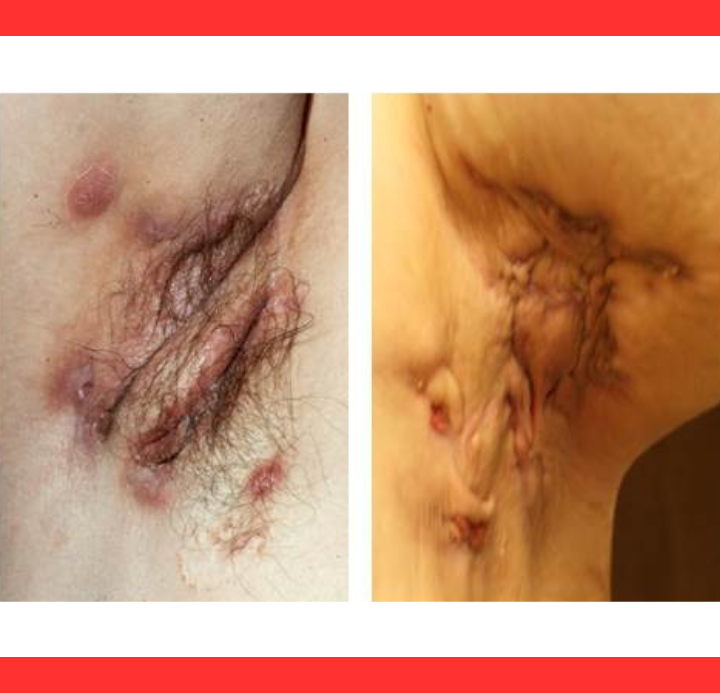
The true horror of HS lies in its subterranean destruction. Before visible lumps surface, inflammation erodes follicular walls, forming sinus tracts—tunnel-like channels that snake beneath the skin.
These hidden pathways link distant abscesses, fostering chronic infection and extensive fibrosis.
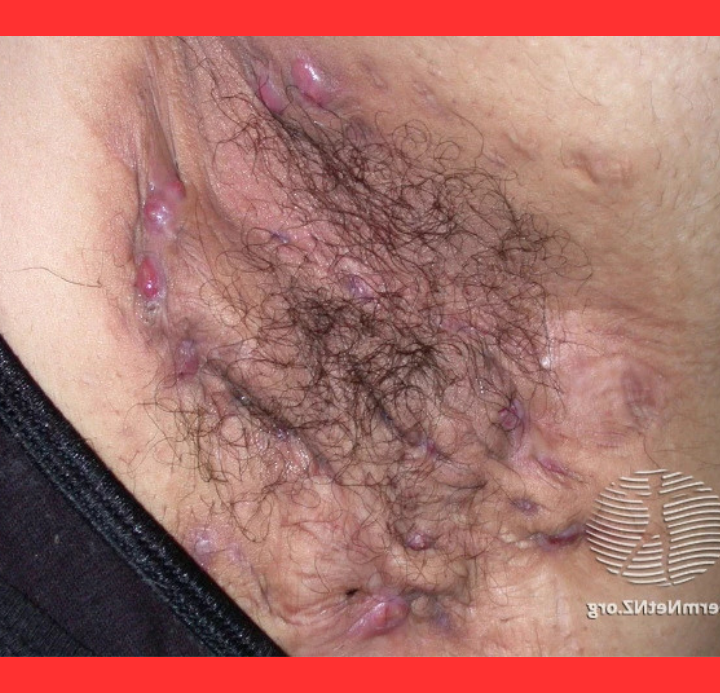
Scar tissue builds internally, distorting anatomy long before external signs fully reveal the damage, explaining why early intervention proves so elusive.
Patients endure not only physical torment but profound emotional strain.
Constant pain limits mobility, while visible scars and odor breed shame and social withdrawal. Many report anxiety, depression, and strained relationships, as intimate areas bear the brunt.
Daily activities like walking or wearing fitted clothes become ordeals, silently eroding confidence and mental health.
Diagnosis frequently takes a decade or more, as initial symptoms mimic boils, cysts, or sexually transmitted infections.
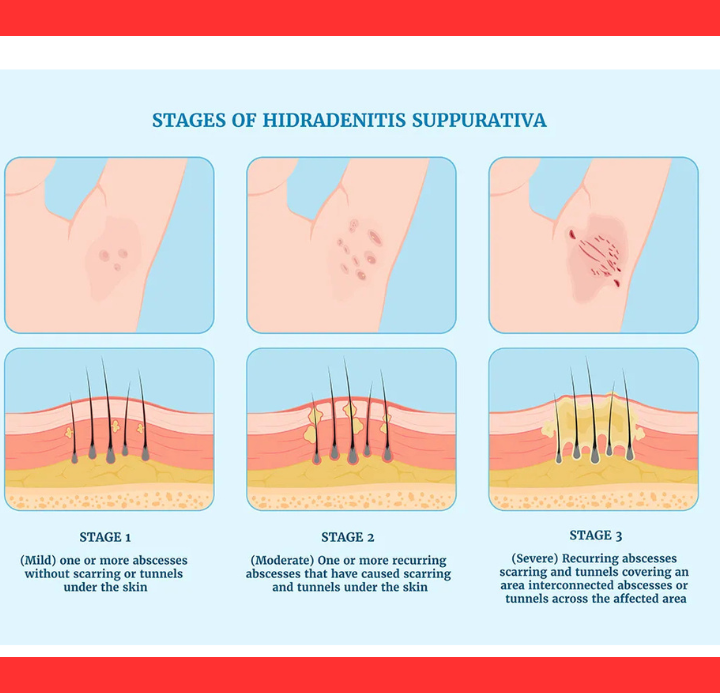
Dermatologists rely on clinical history and the Hurley staging system to classify severity—from isolated nodules in Stage 1 to widespread tunnels and scarring in Stage 3.
Biopsies or imaging occasionally confirm the extent of internal involvement, yet awareness gaps among physicians prolong suffering.
Medical management focuses on reducing inflammation and preventing flares.
Topical or oral antibiotics combat secondary infections, while biologic drugs like adalimumab target the immune overdrive.
Anti-inflammatory medications and hormonal therapies offer relief for some.
For advanced cases, surgical removal of affected tissue or laser therapy provides lasting improvement, though recurrence remains possible without ongoing care.
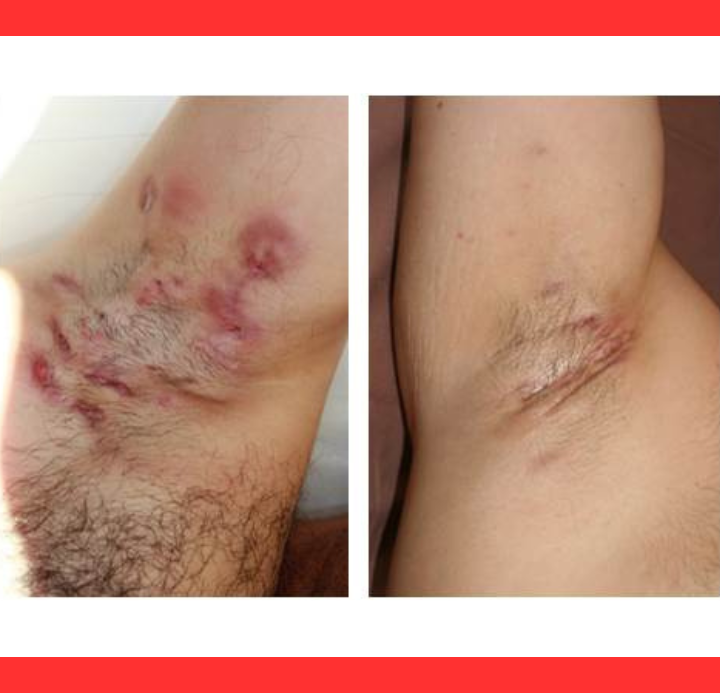
Lifestyle changes prove essential alongside treatment.
Quitting smoking dramatically reduces flare frequency, and weight loss eases friction in skin folds.
Gentle cleansing, loose clothing, and warm compresses help manage symptoms at home.
Support groups and specialized clinics empower patients, fostering hope that proper management can halt progression and restore normalcy.
Raising awareness about hidradenitis suppurativa is crucial to end the silence surrounding this invisible destroyer.
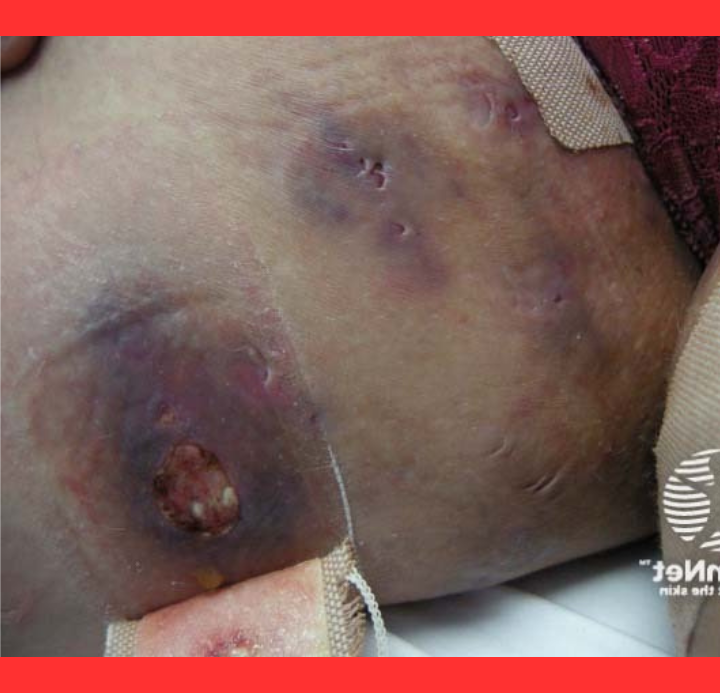
Early recognition and multidisciplinary care can prevent devastating scarring and improve lives dramatically.
If painful lumps persist in friction-prone areas, consulting a dermatologist promptly offers the best path forward toward control and healing.
